How aggressively should psoriasis in a teenager be treated?
She’s in her late teens. Reserved, and guarded with her answers.
I was trying to work out if she was having any symptoms or signs related to psoriatic arthritis. I worked through my questions on joints, then tendons, then tendon attachments, followed by the spine.
There were none.
So, the reason she went to a GP practice and requested a referral to a “joint” doctor, when she did not have any issues with her joints, ligaments or tendons?
Bad skin.
She showed me the areas she had tried to cover up and I looked at the usual sites where I would expect to see psoriasis.
And I had to agree she had what I would also call bad skin. In fact, very bad skin.
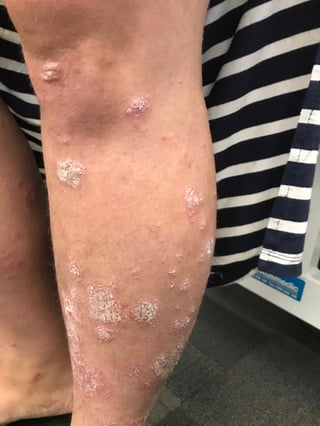
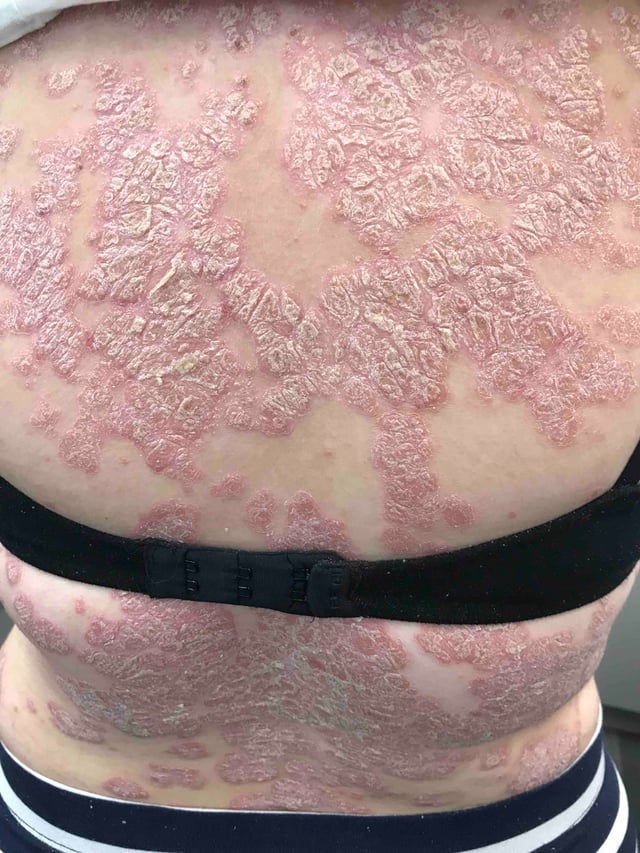
My teenage daughter will obsess over a pimple on her face. I know I’ve been embarrassed and worried about my own skin breakouts.
So, it must be so difficult for a teenager (actually, anyone) to cope with psoriasis of this degree.
She has seen a number of GPs as well as two dermatologists. A variety of creams, ointments and concoptions have been trialled without any response. No other medication suggestions had been made by the doctors.
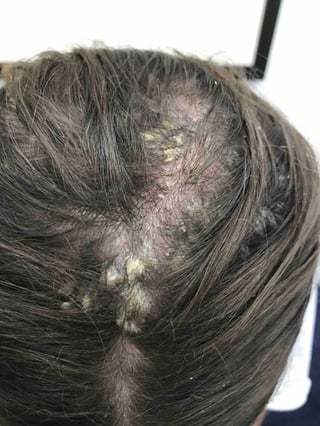 Psoriasis affecting the scalp
Psoriasis affecting the scalp
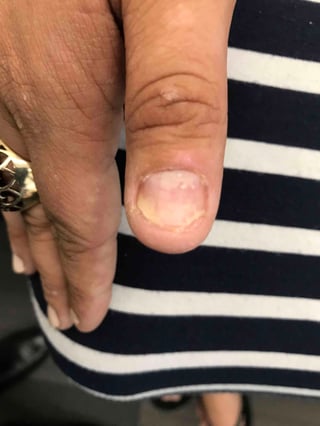 Nail changes seen in Psoriasis
Nail changes seen in Psoriasis
Through the internet, she learned about biologic DMARDs. So she booked in to see me to talk about these.
I do think she will respond and probably needs these agents. The difficulty is that she does not currently qualify for these medications within our regulatory system.
I’ve commenced her on Methotrexate as a starting point. Methotrexate can help with the skin and nail disease, and it may help prevent the joint manifestations she is at risk of.
I plan to refer her on to a more sympathetic and “aggressive” dermatologist as she needs the very best options available.

